Dr. Taylors Recipe For Gum Health
Use a Water-Pik or other oral irrigator to irrigate every day with diluted Saturated Salt Solution.
To make saturated salt solution:
• Get a large glass jar: (1 or 2-quart size). Mason jars are ideal.
• Put about ½ an inch of baking soda and ½ an inch of salt in the bottom of the jar.
• Fill the jar with very warm water.
• Turn the jar over a few times to mix it up.
• Let the solution settle for 8 or more hours.
• The clear part above the silt is Saturated Salt Solution.
• Don’t get the silt in your irrigator. It’ll get clogged.
Each Day:
In a new container, dilute the solution with one part warm water and one part solution. Don’t stir up the silt when you pour it off. The silt will clog your WaterPik. Irrigate all around every one of your teeth with a gentle, low pressure setting. Run tap water through your waterpik afterward to keep it clean.
These recommendations are based on research summarized in:
EFFICIENT ANTIMICROBIAL TREATMENT IN PERIODONTAL MAINTENANCE CARE
JØRGEN SLOTS, D.D.S., D.M.D., PH.D., M.S., M.B.A. and MICHAEL G. JORGENSEN, D.D.S.
J Am Dent Assoc, Vol 131, No 9, 1293-1304.
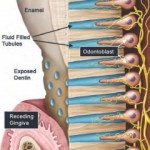
 I have spent a lot of time researching and thinking about dental recalcification, so I was drawn to this book Heal Tooth Decay by Ramiel Nagel. Here are my thoughts on Nagel’s influential and informative book. The short of it: the book tells the truth as the author’s encountered it. Does its advice work for some? Yes. It doesn’t work for everyone though. I want it to, but it doesn’t.
I have spent a lot of time researching and thinking about dental recalcification, so I was drawn to this book Heal Tooth Decay by Ramiel Nagel. Here are my thoughts on Nagel’s influential and informative book. The short of it: the book tells the truth as the author’s encountered it. Does its advice work for some? Yes. It doesn’t work for everyone though. I want it to, but it doesn’t.